Penicillin Allergy Guide: Safety, Testing, and Managing Your Risks

Quick Takeaways
- Most reported penicillin allergies are actually side effects or outdated reactions.
- True allergies are categorized as immediate (IgE-mediated) or delayed.
- Skin tests and oral challenges can safely remove an allergy label for most people.
- Mislabeling increases the risk of antibiotic-resistant infections like MRSA.
- High-risk patients must avoid these drugs in non-emergency settings.
Spotting the Difference: Side Effects vs. True Allergies
Not every bad experience with a pill is an allergic reaction. Many people remember a stomach ache or a mild headache after taking Amoxicillin as a child and assume they are allergic. In reality, these are side effects or intolerances, not immune responses. True allergies are usually split into two camps: immediate and delayed. Immediate reactions happen within an hour. These are the scary ones, often driven by IgE antibodies, which can lead to Anaphylaxis a severe, potentially life-threatening systemic allergic reaction. If you've ever experienced your throat closing, your tongue swelling, or a sudden drop in blood pressure after a dose, you're in the high-risk category. Delayed reactions are a different beast. They can show up hours or even days later. You might see a maculopapular rash (small red bumps) appearing 72 to 96 hours after the first dose. In rare, severe cases, this can escalate to conditions like Stevens-Johnson Syndrome, where the skin blisters and peels. Because these don't happen instantly, people often don't connect them to the medication until much later.Who Is Actually at Risk?
Doctors now use risk stratification to decide if you can safely take a certain drug or if you need a specialist. You generally fall into one of three buckets:- Low Risk: You had a mild rash years ago, or you just remember "feeling sick" (nausea, headache) after the medicine. Most people in this group can safely take first-generation Cephalosporins (like cefazolin) without any extra testing.
- Moderate Risk: You had hives, facial swelling, or respiratory distress, but it wasn't a full-blown collapse. These patients usually need a formal allergy test before trying any beta-lactams.
- High Risk: You've had anaphylaxis in the last 10 years or suffered from severe organ-specific reactions (affecting the liver or kidneys). These individuals should never take penicillin in a standard clinic or home setting; they need a controlled hospital environment and an allergist.
| Risk Category | Common Symptoms | Recommended Action |
|---|---|---|
| Low | Nausea, mild rash, remote childhood reaction | Safe for many cephalosporins; low-risk for challenge |
| Moderate | Hives, angioedema, respiratory distress (>5 years ago) | Requires skin testing or supervised challenge |
| High | Recent anaphylaxis, SJS/TEN, organ failure | Avoid beta-lactams; refer to specialist |
The Process of "De-Labeling" Your Allergy
If you're tired of getting the "alternative" antibiotic that doesn't work as well, you can ask your doctor about de-labeling. This is the process of proving you aren't allergic so the warning can be removed from your medical record. It usually starts with a skin test. Doctors use "major and minor determinants"-basically small amounts of the drug-to see if your skin reacts. If the skin test is negative, the next step is an observed oral challenge. You'll take a small dose (often 250 mg of amoxicillin) while a medical professional monitors your vitals for about an hour. Why go through this? Because if both tests are negative, your risk of a severe reaction is virtually zero-the same as someone who never reported an allergy. Once you pass, the doctor documents the challenge in your file. This is a huge win for your long-term health, as it opens up the most effective first-line treatments for future infections.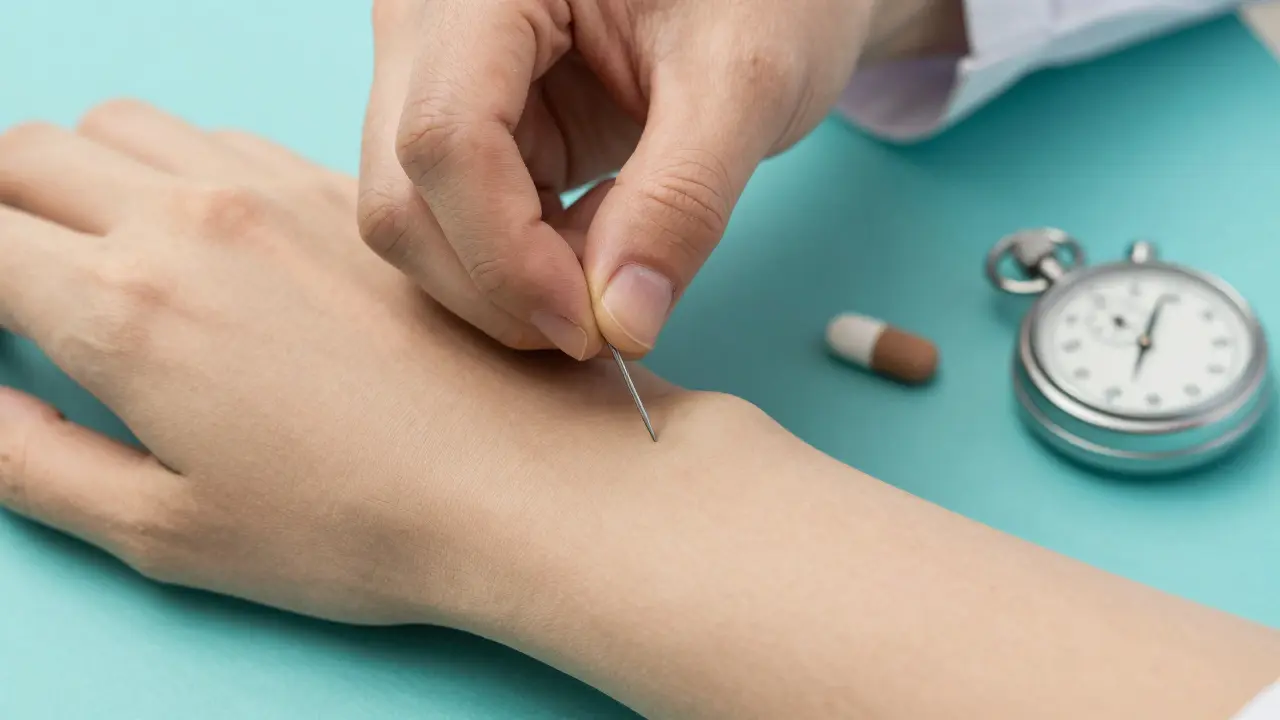
Why an Incorrect Label Is Dangerous
You might think, "Why does it matter if I take a different antibiotic as long as it works?" The problem is that penicillin-type drugs (known as Beta-lactams a class of antibiotics that contain a beta-lactam ring in their molecular structure) are often the most effective tool for the job. When doctors avoid these because of a suspected allergy, they often prescribe "broader-spectrum" antibiotics. These are like using a sledgehammer to crack a nut. They kill the bad bacteria, but they also wipe out the good bacteria in your gut. This creates a breeding ground for Clostridioides difficile (C. diff), a nasty infection that causes severe diarrhea. Moreover, overusing these heavy-duty alternatives contributes to Antimicrobial Resistance. Research shows that people with penicillin allergy labels have significantly higher rates of MRSA (methicillin-resistant Staphylococcus aureus). By incorrectly labeling yourself as allergic, you're actually making it harder for doctors to treat you if you get a serious infection later.Staying Safe: Your Action Plan
Whether you have a confirmed allergy or just a suspicion, your safety depends on clear communication. First, make sure your medical records are accurate. If you've been tested and found *not* to be allergic, ensure that the "allergy" flag is removed from your electronic health record. If you are truly high-risk, a medical alert bracelet is a lifesaver. In an emergency-like a car accident where you're unconscious-paramedics need to know not to give you certain medications. If you're currently undergoing a supervised challenge, your healthcare provider should have an "allergy kit" ready. This isn't just a band-aid; it's a set of emergency meds including Epinephrine, diphenhydramine, and hydrocortisone. If you're at home and experience sudden swelling of the lips or difficulty breathing after a new medication, don't wait. Call emergency services immediately.
Looking Ahead: The Future of Allergy Management
Medical systems are moving toward a more proactive approach. Many hospitals are now implementing formal de-labeling programs. By systematically identifying patients who are likely mislabeled, some facilities have removed incorrect allergy labels from up to 90% of eligible patients. By 2025, it's expected that half of all U.S. hospitals will have these protocols in place. This shift doesn't just save the healthcare system money-it's estimated to save over $1 billion annually-but it prevents surgical site infections and reduces hospital stays. The goal is simple: getting the right drug to the right patient without unnecessary fear.Can I take cephalosporins if I'm allergic to penicillin?
It depends on your risk level. Low-risk patients (those with mild or remote reactions) can often safely take first-generation cephalosporins like cefazolin. However, those with a history of anaphylaxis or severe skin reactions should avoid them until they are cleared by an allergist, as there is some cross-reactivity between these drug classes.
How long does a penicillin allergy last?
It varies by the type of reaction. About 80% of people with an IgE-mediated (immediate) allergy lose their sensitivity after 10 years without exposure. Delayed reactions, such as mild rashes, often disappear even faster, sometimes within 1 to 2 years.
What should I do if I suspect I'm allergic to penicillin?
Start by documenting exactly what happened: What was the drug? When did the reaction start? What were the symptoms? Take this information to your primary care doctor or an allergist. They can determine if you are low, moderate, or high risk and decide if a skin test or oral challenge is appropriate for you.
Is a "skin prick test" enough to prove I'm not allergic?
A skin test is a great first step, but for a definitive answer, doctors usually follow a negative skin test with an oral challenge. When both are negative, the risk of anaphylaxis is considered nearly zero, allowing the doctor to safely remove the allergy label from your record.
What are the signs of a severe penicillin reaction?
Immediate severe reactions include swelling of the tongue, throat, or lips, difficulty breathing, a sudden drop in blood pressure, and loss of consciousness. Delayed severe reactions can include widespread skin peeling, blistering, or high fever accompanied by organ dysfunction. Both require immediate emergency medical attention.
