Menopause Weight Gain: Hormones, Muscle, and Strategy

You wake up one morning, step onto the scale, and the number is higher. You haven't changed what you eat. You're walking the dog just as much. Yet, your waistline has shifted. This is a common story for women entering the menopausal transition, but the reasons are far more complex than "eating too much." When women reach perimenopause, their bodies undergo a fundamental biological reorganization that prioritizes abdominal fat storage over subcutaneous fat. Understanding the mechanics behind this shift is the first step toward managing it.
Menopause weight gain is defined as the physiological accumulation of body fat, particularly around the abdomen, occurring during the menopausal transition due to hormonal fluctuations and aging. According to the long-running Study of Women's Health Across the Nation (SWAN)a longitudinal study by the National Institutes of Health tracking women's health, women typically gain approximately 1.5 kilograms per year during perimenopause. This isn't random; it is driven by a specific cascade of hormonal and metabolic events that alter how your body processes energy.
The Hormonal Mechanics of Weight Gain
The primary driver of this change is the sharp decline in estrogen production. Specifically, estradiol levels can drop by roughly 60-70% during the transition. In premenopausal years, Estradiolthe primary form of estrogen in women, crucial for regulating metabolism and fat distribution helps maintain a healthy balance between fat and muscle. When levels fall from typical ranges of 70-150 pg/mL down to 10-20 pg/mL, the body loses a key regulator of appetite and fat storage.
This shift triggers a domino effect involving other hormones. Leptin, the hormone that tells your brain you are full, sees a production reduction of 20-30%. Simultaneously, ghrelin, the hunger hormone, rises by about 15-25%, largely because sleep disruptions from hot flashes interrupt rest cycles. This means your body is biologically signaling hunger even when you are eating normally. Many women report feeling constantly hungry despite maintaining their previous calorie intake. This hormonal mismatch makes traditional dieting ineffective because the body is fighting for fuel it perceives as scarce.
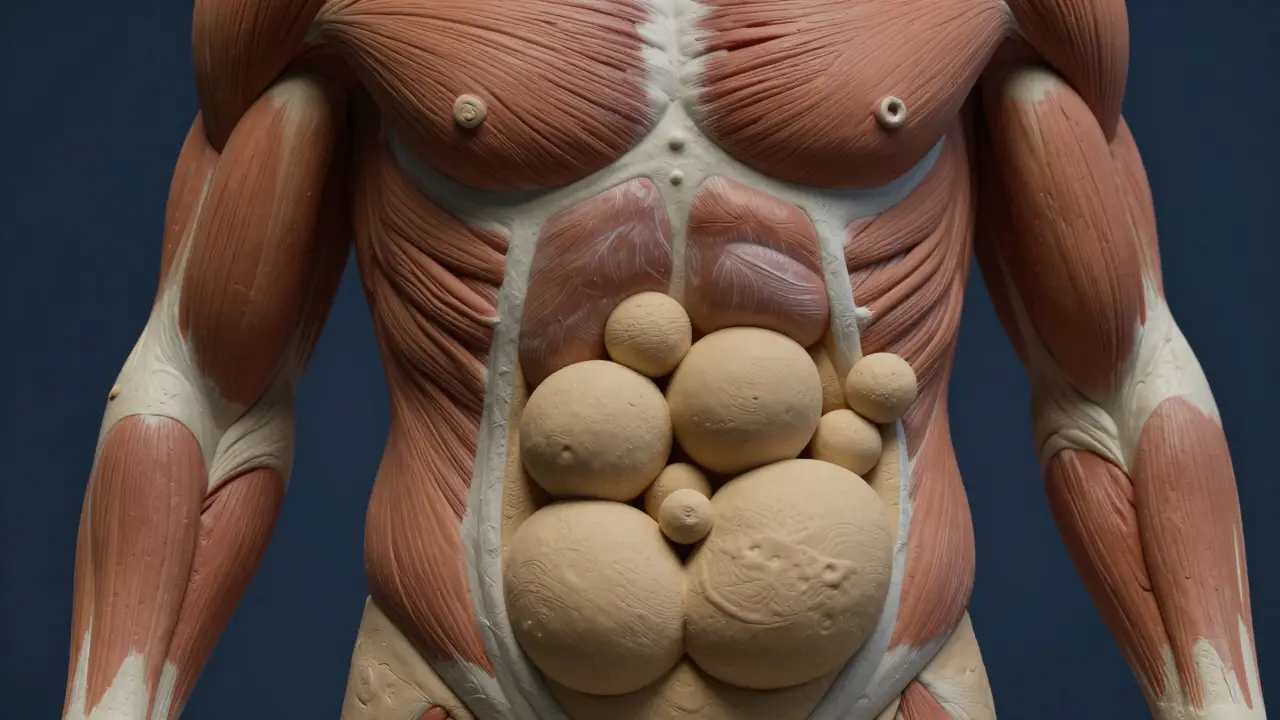
Beyond appetite, the hormonal profile shifts toward a relative increase in testosterone. While testosterone exists in lower amounts in women, the ratio changes as estrogen drops. This contributes significantly to why fat moves from the hips and thighs to the belly. It is not simply extra fat; it is stored differently. Postmenopausal women experience a 25-35% shift toward abdominal fat storage. This is dangerous because abdominal fat is metabolically active tissue.
The Role of Muscle Loss and Metabolism
While hormones get the blame, muscle loss plays an equally critical role. As we age, we naturally lose lean muscle mass, a process known as sarcopenia. Typically, women lose 3-8% of lean muscle mass per decade after age 30. However, menopause accelerates this rate by an additional 1-2% annually. Since muscle burns more calories at rest than fat does, losing muscle directly reduces your resting metabolic rate by approximately 2-3% per decade.
This creates a double burden: you burn fewer calories while simultaneously craving more energy due to leptin resistance. Clinical analysis from Dr. Stephanie Faubion, medical director of The Menopause Society, indicates that this metabolic slowdown often persists regardless of caloric intake. Simply cutting calories without addressing muscle preservation leads to further metabolic damage. Your body adapts to the deficit by holding onto fat reserves, making sustained weight loss frustratingly slow. On average, postmenopausal women lose weight at 20-30% slower rates than their premenopausal counterparts at the same caloric deficit.
Visceral Fat and Health Risks
It is vital to understand that the location of the weight matters more than the number on the scale. Premenopausal women store 60-70% of body fat subcutaneously, meaning under the skin on the legs and glutes. After menopause, 45-55% of new fat deposits accumulate in the visceral abdominal region. Visceral fatfat stored deep within the abdominal cavity surrounding organs like the liver and intestines acts almost like an active endocrine organ. It releases inflammatory cytokines at 3-5 times the rate of subcutaneous fat.
This inflammation increases insulin resistance by 20-40%, raising the risk of type 2 diabetes. Beyond blood sugar control, the cardiovascular risk skyrockets. Research shows postmenopausal women are nearly five times more likely to develop abdominal obesity compared to premenopausal women. Dr. Mary Jane Minkin, a clinical professor at Yale University, warns that this shift increases cardiovascular risk by 25-30% independent of overall BMI. A woman can have a "normal" BMI but carry dangerous levels of visceral fat that threatens heart health.
| Feature | Premenopausal Status | Postmenopausal Status |
|---|---|---|
| Fat Storage Location | Hips, Thighs, Buttocks (Subcutaneous) | Abdomen, Organs (Visceral) |
| Estrogen Levels | 70-150 pg/mL | 10-20 pg/mL |
| Metabolic Rate | Stable to Moderate Decline | Rapid Decline (-2-3% per decade) |
| Muscle Retention | Natural Aging Loss | Accelerated Loss (+1-2% annually) |
| Cardiovascular Risk | Standard | Increased by 25-30% |
Exercise Strategies for Muscle Preservation
If muscle loss drives the weight gain, the solution must involve building muscle back up. Cardio alone is insufficient for this goal. Walking is excellent for heart health, but it does not stimulate significant muscle growth required to offset sarcopenia. The most effective protocol involves resistance training performed 2-3 times weekly combined with high-intensity interval training (HIIT) 1-2 times weekly.
A randomized controlled trial published in *Menopause: The Journal of The North American Menopause Society* demonstrated that this combination increases lean muscle mass by 1.8-2.3 kg over six months. It also reduces abdominal fat by 8-12%. Consistency is key here. You do not need heavy weights to start, but progressive overload-increasing resistance or repetitions over time-is necessary. Compound movements like squats, lunges, and rows engage multiple muscle groups, maximizing hormonal response and calorie burn during the session and recovery period.
Nutritional Adjustments for the Changing Metabolism
Dietary needs change drastically when metabolism slows. Relying on old portion sizes can result in a surplus. More importantly, the quality of protein intake becomes critical. Age-related anabolic resistance means your body struggles to utilize protein for muscle repair unless intake is sufficient. The British Menopause Society recommends a protein intake of 1.2-1.6 grams per kilogram of body weight daily.
To achieve this practically, aim for 25-30 grams of protein per meal. For a 60kg woman, this translates to roughly 1000mg of protein spread across three meals plus snacks. Prioritizing protein early in the day helps blunt glucose spikes and maintains satiety hormones. Additionally, sleep optimization is non-negotiable. Achieving 7-8 hours of quality sleep reduces ghrelin levels by 15-25%. If hot flashes are disrupting sleep, cooling strategies or medical consultation may be necessary before any diet plan can succeed.
Medical Management and Future Options
For some women, lifestyle changes need support from medical interventions. Hormone therapy (HT) remains a powerful tool. By replacing declining estrogen levels, HT can help mitigate the rapid muscle loss and visceral fat accumulation, though it must be tailored to individual risk profiles. Currently, comprehensive menopause management is not always covered by insurance; only 37% of major U.S. health insurers cover these programs fully.
Looking ahead, pharmaceutical options are evolving. The FDA approved bimagrumab for Phase 3 trials in late 2023. As a myostatin inhibitor, it aims to simultaneously increase muscle mass by 5-7% and reduce fat mass by 8-10%. While not yet widely available as of early 2026, these advancements signal a shift toward treating menopause as a distinct metabolic condition rather than just a symptom to endure. Precision medicine is also arriving, with protocols analyzing 17 hormonal and metabolic markers to create personalized weight management plans.
Managing Expectations and Timeline
Patience is arguably the most important component of this strategy. The learning curve for implementing strength training and dietary adjustments typically requires 3-6 months for noticeable results. Frustration often peaks around the four-month mark when the scale stalls. This is normal. Your body is restructuring itself, prioritizing internal health over external size. Working with a healthcare provider for 6-12 months allows for adjustments based on your specific hormonal profile and metabolic responses.
Remember that 78% of women reported unexpected weight gain despite unchanged habits according to Mayo Clinic Connect forums. You are dealing with biology, not willpower. By focusing on muscle preservation, nutrient timing, and realistic timelines, you move from fighting your body to working with its new operational requirements. The goal shifts from simple weight loss to metabolic health and longevity.
Is all weight gain during menopause caused by hormones?
Hormones play a major role, particularly the drop in estrogen, which changes where fat is stored. However, aging-related muscle loss (sarcopenia) and decreased physical activity contribute significantly. Experts often cite the combination of hormonal shifts and lifestyle factors as the primary drivers.
How much protein should I eat daily during menopause?
Current guidelines suggest aiming for 1.2 to 1.6 grams of protein per kilogram of body weight daily. Spreading this into 25-30 gram servings per meal helps combat muscle loss and supports metabolic health.
Does exercise actually stop the weight gain?
Regular resistance training combined with HIIT can reduce abdominal fat by 8-12% and increase muscle mass, which boosts your resting metabolic rate. It is considered the most effective non-pharmaceutical intervention.
What is visceral fat and why is it dangerous?
Visceral fat is fat stored around internal organs. It is metabolically active and produces inflammatory chemicals, increasing the risk of insulin resistance, type 2 diabetes, and cardiovascular disease by up to 30% compared to subcutaneous fat.
Can hormone therapy help with weight management?
Yes, for eligible candidates, hormone therapy can stabilize metabolic shifts associated with low estrogen levels. However, it should be discussed with a specialist to evaluate personal risks regarding cardiovascular health and cancer history.

Victor Ortiz
March 31, 2026 AT 21:29The data presented here is incomplete without considering genetic predisposition markers. Estrogen fluctuation is only part of the equation when analyzing visceral fat distribution patterns. We need to see longitudinal data on cortisol levels to validate these claims properly. It feels like a simplification for a general audience. Scientific rigor is lacking in this summary.
Cameron Redic
April 2, 2026 AT 16:55That is overly sentimental for a medical discussion. Focus on the data points instead of feelings please. People need solutions not emotional validation essays.
RONALD FOWLER
April 4, 2026 AT 00:04Hey Cameron I understand frustration but empathy drives motivation significantly. We need both head and heart to succeed here. Kindness helps retention of information better than harshness. Let us support each other through this tough time.
Amber Armstrong
April 4, 2026 AT 16:00I really feel for anyone reading this and struggling with the scale numbers. It feels so unfair that your body suddenly decides to change rules without warning you first. You do everything right and still see the belly grow around organs instead of hips. The science here explains exactly why that happens though. It helps me stop beating myself up about it constantly. We aren't lazy for gaining weight when our hormones drop off a cliff like that. Muscle loss is just as huge of a factor than what we eat honestly. Walking the dog doesn't fix sarcopenia unfortunately. We need heavy weights and protein to fight that aging process. Sleep matters too when hot flashes keep us up all night every single time. Leptin resistance makes hunger feel like a survival signal rather than actual need. Understanding the biology removes the shame from the experience. It gives us tools to manage it better moving forward. I hope everyone finds gentle ways to adjust their habits. Support groups really help when you know you are not alone. Please take care of your hearts during this transition phase always.
Ruth Wambui
April 6, 2026 AT 08:22They don't tell you about the fluoride impact on the endocrine system either. Big Pharma profits from hormone imbalances and keeps women dependent on drugs. Wake up to the real agenda behind menopause marketing campaigns. Your ovaries are targeted by environmental toxins everywhere.
Carolyn Kask
April 8, 2026 AT 06:05Typical conspiracy noise distracting from actual health data. Get back to reality before you hurt yourself. We need facts not wild theories about water supplies.
Dan Stoof
April 9, 2026 AT 05:42YES!!! YOU GOT THIS WOMEN!!! PROTEIN IS POWERFULLLL!!! Lift those heavy things up NOWWWWW!!! Do not let the metabolism win todayyyy!!!
William Rhodes
April 10, 2026 AT 05:32Passion is good but aggression hurts progress sometimes. Stay positive but check your volume levels too. Hard work beats theory every single time.
Katie Riston
April 12, 2026 AT 03:15Aging is truly the great equalizer we all must face eventually. Menopause forces us to confront the impermanence of our physical forms deeply. There is wisdom in accepting the new metabolic reality calmly. Resisting biology brings suffering while acceptance brings peace often. We are vessels carrying energy through different stages of life. The shift from reproductive prime to preservation mode makes sense evolutionarily. Yet modern society judges us for these natural transitions harshly. Visceral fat is protection mechanism for winter survival instincts now dormant. We must reinterpret what safety looks like for the body now. Emotional regulation might matter more than waist circumference measurements. Health spans are defined by internal balance not external size charts. Every woman carries unique burdens regarding hormonal decline rates. Patience becomes the greatest muscle we can train alongside biceps. Our minds must lead where our bodies follow slowly. Listening to signals of hunger is less important than listening to intuition. I find meaning in surviving the transition rather than conquering it aggressively.
Marwood Construction
April 13, 2026 AT 18:47While poetic, clinical metrics remain the gold standard for assessment. Metabolic efficiency requires quantifiable data to track accurately. Philosophy does not cure insulin resistance issues directly.
Biraju Shah
April 15, 2026 AT 09:24Listen up, you need to move weights or stay sick. Stop waiting for pills to save your metabolic rate now. Action cures stagnation regardless of the hormone numbers. Do the work consistently every single week.
Calvin H
April 16, 2026 AT 16:30Yeah sure just add more protein to my diet like money is free lol.
Brian Yap
April 18, 2026 AT 15:26Mate chuckle fair point about the wallet aspect there. Budget fitness is tricky down here in Australia too. Keep smiling through the struggle.