Eczema vs. Psoriasis: How to Tell the Difference in Your Rash
If you've ever looked at a red patch on your skin and wondered, "Is this just a bad reaction to a soap, or is it something more?" you aren't alone. Distinguishing between Eczema is a chronic, immune-mediated condition often triggered by allergens that causes itchy, inflamed skin and Psoriasis is an autoimmune disorder that speeds up skin cell production, resulting in thick, scaly plaques can be incredibly frustrating. They both cause redness, itching, and scaling, but treating them as if they are the same is a mistake. In fact, research from the Journal of the American Academy of Dermatology shows that about 15-20% of cases are misdiagnosed, which can lead to using the wrong creams and making the inflammation worse.
The good news is that while they look similar at a glance, there are specific "tell-tale" signs that can help you figure out what you're dealing with. Whether you're noticing a rash in the crook of your arm or a thick patch on your knee, the key is looking at the borders, the texture, and exactly where on the body the rash likes to hang out.
Where the Rash Hits: Flexors vs. Extensors
One of the fastest ways to tell these two apart is by looking at the location. Dermatologists often use a simple rule: eczema loves the creases, while psoriasis loves the outer edges. In medical terms, these are called flexural and extensor surfaces.
If you have eczema, you'll likely find the rash on your flexural surfaces. Think of the areas that fold: the inner elbows, behind the knees, the wrists, and the ankles. In children, it's very common to see these patches on the cheeks. According to clinical reviews, about 92% of eczema cases affect the inner elbows. It's like the skin is reacting to the friction and moisture trapped in those folds.
On the flip side, Psoriasis usually targets the extensor surfaces-the parts of your joints that stretch. This means the outer elbows, the front of the knees, and the scalp. If you see a thick patch right on the point of your elbow or the top of your knee, there's a much higher chance it's psoriasis. While there is a version called "inverse psoriasis" that shows up in skin folds, it usually looks smooth and shiny rather than scaly, which is a big clue that it's different from typical eczema.
Analyzing the Texture: Weepy vs. Armor-Plated
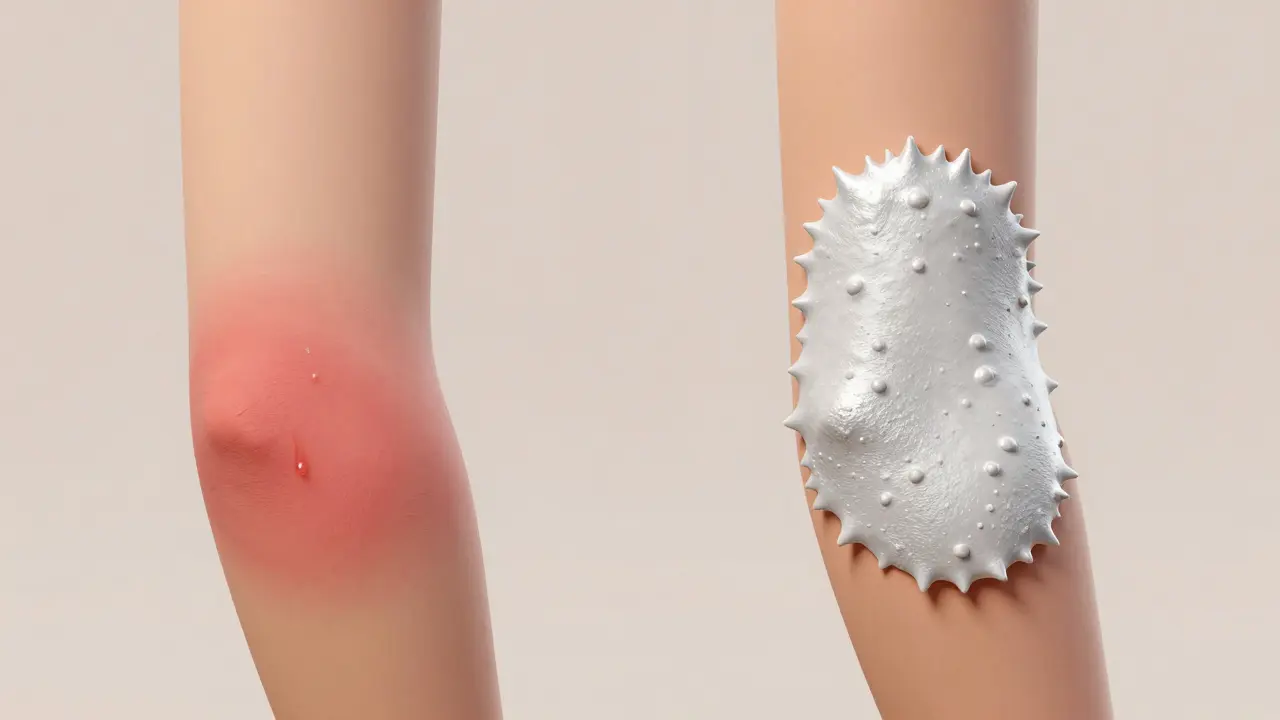
If you look closely at the rash, the texture tells a different story. Eczema is often "messy." It usually presents as poorly defined patches that blend into the surrounding skin. In an active flare-up, you might see oozing or crusting-what doctors call exudative characteristics. The skin often looks raw and can crack easily because the skin barrier is compromised.
Psoriasis is much more "defined." The most common form, Plaque Psoriasis is a type of psoriasis characterized by raised, red patches covered with a silvery-white scale , creates borders that are very clear. Instead of oozing, psoriasis looks dry. Many patients describe it as feeling like "armor plating." These scales are significantly thicker than the fine scaling found in eczema-averaging about 0.5mm compared to just 0.1mm for eczema.
| Feature | Eczema (Atopic Dermatitis) | Psoriasis (Plaque) |
|---|---|---|
| Borders | Blurred, blends into skin | Well-defined, sharp edges |
| Scale | Fine, thin scaling | Thick, silvery-white scales |
| Surface | Often weepy, oozing, or raw | Dry, thick, "plaque-like" |
| Location | Inner elbows, back of knees | Outer elbows, front of knees, scalp |
The Challenge of Skin of Color
It is vital to realize that the "classic red rash" described in old textbooks doesn't apply to everyone. If you have a medium to dark skin tone (Fitzpatrick skin types IV-VI), these conditions can look completely different, which unfortunately leads to longer diagnostic delays-sometimes over 14 months longer than for white patients.
For someone with darker skin, eczema might not look red at all. Instead, it often appears as ashen, purple, or gray patches. You might see hyperpigmented (darker) or hypopigmented (lighter) areas with very subtle scaling. Psoriasis on darker skin often shows up as violaceous (purple) or dark brown patches. One unique marker for psoriasis in skin of color is a "halo" of lighter skin around the active lesion, a trait rarely seen in eczema.
Beyond the Rash: Nails and Trauma
If you're still unsure, look at your nails and think about how the rash started. Psoriasis often leaves a trail beyond the skin. About 50% of people with psoriasis experience "nail pitting," which are tiny pin-sized depressions in the nail plate. You might also notice onycholysis, where the nail actually starts to separate from the nail bed. Eczema almost never causes this kind of nail damage.
Then there is the Koebner Phenomenon is a skin reaction where new psoriasis lesions form at the site of an injury or trauma . If you scratch your arm or get a small cut, and a new psoriasis plaque forms exactly where the injury happened, that's a huge diagnostic clue. This rarely happens with eczema.
Practical Ways to Track Your Skin
While you should always see a professional for a final diagnosis, you can gather better data for your doctor by tracking your flares. Psoriasis plaques tend to be more stable-they stay looking like plaques for a while. Eczema, however, is a shapeshifter. It fluctuates wildly based on triggers like a new laundry detergent, a stressful week, or a change in weather.
Try taking photos of your lesions under the same lighting every few days. Note if the rash is oozing or if it's purely dry. If you're brave enough to try a "scale test" (as suggested by Mayo Clinic guidelines), gently scraping a lesion with a glass slide can be telling. Psoriasis scales often reveal tiny pinpoint bleeding points when removed-known as the Auspitz sign-whereas eczema scales do not.
Can I have both eczema and psoriasis at the same time?
Yes, it is possible to have both, although it's less common. This is sometimes called "psoriasiform dermatitis." Because both are inflammatory conditions, they can coexist, but they will usually maintain their distinct visual characteristics (e.g., some patches will be weepy and in the creases, while others are thick and on the elbows).
Does one itch more than the other?
Generally, eczema is known for an intense, almost unbearable itch that often leads to scratching and further skin damage (lichenification). Psoriasis can also itch or feel like a burning sensation, but the primary characteristic is often the thickness and tightness of the skin rather than the frantic itch associated with eczema.
Will over-the-counter creams work for both?
Some mild steroid creams may reduce inflammation for both, but the long-term approach is different. Eczema requires a heavy focus on barrier repair and avoiding triggers. Psoriasis often requires medications that slow down the rapid production of skin cells. Using the wrong approach can sometimes lead to skin thinning or ineffective treatment.
How can I tell if my rash is just a simple allergic reaction?
Allergic contact dermatitis often looks like acute eczema-red, itchy, and sometimes weepy. The main difference is the timing and location. Allergic reactions usually appear quickly after contact with a specific substance (like a new fragrance) and disappear once the trigger is removed. Eczema and psoriasis are chronic, meaning they flare and remit over years.
Are AI skin apps accurate for diagnosis?
Some AI tools have reached around 85% accuracy in clinical settings, but they aren't perfect. They struggle significantly more with skin of color, where accuracy can drop by over 20%. They are great for tracking changes or getting a "hunch," but you should never use them to replace a physical exam by a dermatologist.
What to Do Next
If your rash is spreading, causing you to lose sleep, or showing signs of infection (like yellow crusting or warmth), it's time to book an appointment. To make the most of your visit, bring a list of your current soaps and lotions, and show the doctor the photos you've taken of your flares over the last few weeks.
If you have a darker skin tone, don't be afraid to ask your provider specifically how these conditions present in your skin type. Since many medical textbooks still focus on lighter skin, being your own advocate helps ensure you get the right diagnosis faster.

Michael Lewis
April 16, 2026 AT 13:46Actually getting a pro diagnosis is the only way to go. Don't let the internet fool you into thinking a quick checklist is enough. Get to a derm and get it sorted so you can feel better! 💪✨
Joshua Nicholson
April 17, 2026 AT 09:19idk man feels like a lot of this is just common sense if you've ever had a rash before lol
Randall Barker
April 17, 2026 AT 10:31The failure of the medical establishment to properly diagnose people of color isn't just a 'challenge,' it's a moral bankruptcy of the highest order. We live in a society that prizes the aesthetic of the majority while ignoring the visceral suffering of the minority. It is a profound philosophical tragedy that a person's skin tone determines the speed of their healing. We must demand a total systemic overhaul of dermatological education because anything less is an admission that some lives are simply valued less than others. This isn't just about rashes; it's about the inherent dignity of the human being and the right to be seen. If we cannot even agree that a purple patch on dark skin deserves the same urgency as a red patch on light skin, then we have failed as a civilized species. The arrogance of the textbook is the arrogance of the empire. It's honestly disgusting that this is still a talking point in the modern era. We should be ashamed of ourselves for allowing this gap to exist for so long while people suffered in silence. True justice in healthcare isn't just providing a clinic; it's providing a gaze that recognizes all humanity. This is a systemic erasure of the other. We need to stop pretending that 'training' is the solution and start admitting that bias is the engine. The medical field is just another mirror of our fractured social hierarchy. Absolutely pathetic.