Ankylosing Spondylitis Guide: Managing Spine Inflammation and Mobility

Imagine waking up at 4 AM with a back that feels like it has been fused into a solid block of concrete. For people living with Ankylosing Spondylitis is a chronic inflammatory disease that primarily targets the spine and sacroiliac joints, potentially leading to the fusion of vertebrae. While the word "ankylosing" sounds intimidating-and it essentially means "stiffening"-the reality is that early detection and a focused mobility strategy can prevent the dreaded "bamboo spine" and keep you active for decades.
What Exactly Is Ankylosing Spondylitis?
Most people think of back pain as something that happens because you slept wrong or lifted a heavy box. But AS is different. It is a type of Spondyloarthritis, an autoimmune condition where your body mistakenly attacks the entheses-the spots where your ligaments and tendons attach to the bone. Instead of just causing a temporary ache, this inflammation can lead to the growth of new bone, called syndesmophytes, which bridge the gap between vertebrae.
If you are wondering why this happens, genetics play a huge role. There is a strong link to the HLA-B27 gene. While having this gene doesn't guarantee you'll develop the condition, it's present in about 90% of Caucasian patients with AS. However, genetics aren't the whole story; environmental triggers and other biological factors also come into play.
Spotting the Difference: Inflammatory vs. Mechanical Pain
One of the biggest hurdles in treating AS is the misdiagnosis. Many people spend years being told they just have a "bad back" or are stressed, when in reality, they are dealing with systemic inflammation. The key is recognizing that inflammatory pain behaves the opposite of mechanical pain.
Mechanical pain usually gets worse when you move and feels better when you lie down. Inflammatory back pain, however, usually improves with movement and gets worse with rest. If you find that a morning walk actually eases your stiffness but sitting at a desk for four hours makes it unbearable, that is a major red flag. Furthermore, nocturnal pain-specifically the kind that wakes you up between 3 AM and 6 AM-is a classic hallmark of AS.
| Feature | Ankylosing Spondylitis (Inflammatory) | Mechanical Back Pain |
|---|---|---|
| Effect of Rest | Pain increases/Stiffness persists | Pain typically decreases |
| Effect of Exercise | Pain and stiffness improve | Pain often worsens |
| Morning Stiffness | Lasts more than 30 minutes | Brief or non-existent |
| Pain Onset | Insidious (gradual), usually before age 45 | Often sudden (injury) |
The Path to Diagnosis: Beyond the X-Ray
For a long time, doctors relied almost exclusively on X-rays to find Sacroiliitis (inflammation of the sacroiliac joints). The problem is that X-rays only show damage after it has already happened. By the time a "bamboo spine" appears on an X-ray, the fusion is already permanent.
Modern medicine has shifted toward MRI as the preferred early-detection tool. An MRI can spot inflammation and bone marrow edema long before any structural changes are visible. This gap is critical because the goal of current treatment is to stop the inflammation *before* it turns into bone. If you have chronic pain and the HLA-B27 marker, pushing for an MRI rather than just a standard X-ray can be a game-changer for your long-term mobility.
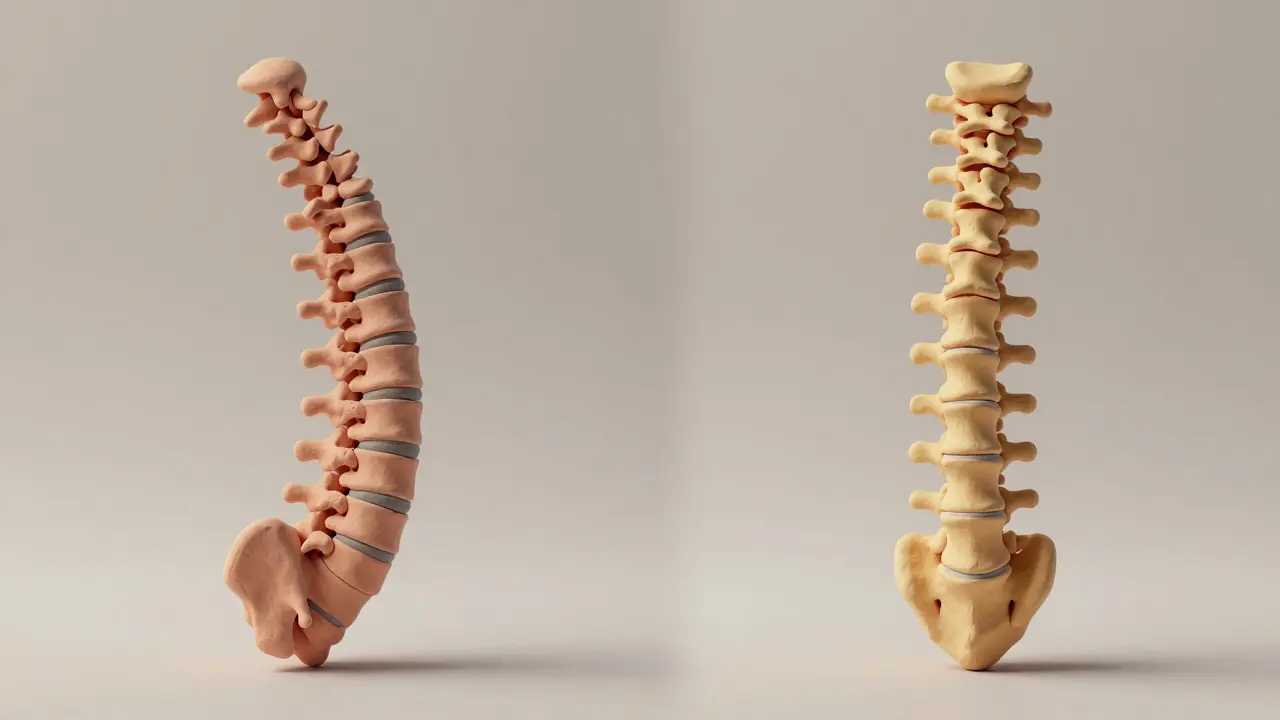
Strategies for Maintaining Spinal Mobility
You cannot "cure" AS, but you can absolutely manage it. The goal is to maintain the range of motion in your spine and chest. When the spine fuses, it doesn't just affect your back; it can limit your ability to breathe deeply if the rib cage loses flexibility.
A successful mobility strategy usually involves three pillars:
- Aquatic Therapy: Swimming is often the gold standard for AS. The buoyancy of the water removes the gravitational pressure on the joints, allowing you to stretch and move your spine in ways that would be too painful on land. Some patients report reducing their morning stiffness from 90 minutes down to 20 minutes just by incorporating daily swimming.
- Spinal Extension Exercises: Focus on movements that keep the spine upright and open. Avoid activities that encourage "slouching" or rounding the back, as this can actually encourage the spine to fuse in a forward-leaning position.
- Deep Breathing: Since AS can affect the joints where the ribs meet the spine, focused diaphragmatic breathing helps keep the chest wall flexible and maintains lung capacity.
The trick is consistency. Research shows that patients using digital tracking tools to monitor their exercises have much higher adherence rates over six months. Start your day with gentle movements while still in bed to "grease the joints" before you even stand up.
Medication and Advanced Therapies
Exercise is vital, but for many, it isn't enough to stop the biological drive toward fusion. This is where pharmacological intervention comes in. The first line of defense is usually NSAIDs (non-steroidal anti-inflammatory drugs). When used correctly, these don't just mask pain; they can actually slow down the radiographic progression of the disease.
When NSAIDs aren't enough, rheumatologists often turn to TNF inhibitors. These are biologic drugs that block the proteins responsible for the inflammatory response. Clinical data suggests that 40-60% of patients see a significant improvement in symptoms within 12 weeks of starting biologics. More recently, JAK inhibitors and IL-17 inhibitors have entered the market, providing alternatives for those who don't respond well to TNF blockers.
It is worth noting that these advanced therapies are expensive and can increase the risk of certain infections. However, the trade-off is often a significant reduction in the likelihood of complete spinal fusion, allowing patients to maintain functional independence well into their later years.

Dealing with the "Whole Body" Impact
AS rarely stays confined to the spine. Because it is a systemic autoimmune disease, it can strike other parts of the body. About a third of patients experience acute anterior uveitis-a sudden, painful inflammation of the eye that requires immediate medical attention to prevent vision loss.
Additionally, there is a surprising link between AS and gut health. Up to 50% of AS patients may develop Inflammatory Bowel Disease (IBD), such as Crohn's or ulcerative colitis. If you have AS and start noticing digestive issues, it's not just a coincidence; it's part of the same inflammatory spectrum. Addressing the gut can sometimes help manage the systemic inflammation affecting the joints.
Daily Living and Ergonomic Adjustments
Beyond the gym and the pharmacy, your environment plays a huge role in how you feel. Small changes to your daily setup can reduce the cumulative strain on your sacroiliac joints.
- Sleep Surface: Ditch the overly soft memory foam. A firm mattress provides the necessary support to keep the spine neutral and prevents the "sinking" feeling that can make morning stiffness worse.
- Workstation Setup: Use a lumbar support cushion. If you work a desk job, consider a standing desk or a chair that encourages an upright posture to counteract the tendency to lean forward.
- Heat Therapy: Applying heat for 20 minutes before your exercise routine can loosen the muscles and make your stretching sessions more effective and less painful.
Can Ankylosing Spondylitis be cured?
No, there is currently no cure for AS, as it is a chronic autoimmune condition. However, it can be managed very effectively. With a combination of biologic medications (like TNF inhibitors) and structured physical therapy, many people live active, productive lives and prevent their spine from fusing completely.
Does the HLA-B27 gene mean I definitely have AS?
Not necessarily. While the HLA-B27 gene is found in the vast majority of AS patients, many people carry the gene and never develop the disease. The gene is a marker that helps doctors with the diagnosis, but they must also look for clinical symptoms like inflammatory back pain and imaging evidence of sacroiliitis.
What is a 'Bamboo Spine'?
A "bamboo spine" is a radiographic term used when the vertebrae have fused together due to the formation of syndesmophytes (bony growths). This makes the spine look like a continuous stalk of bamboo on an X-ray. This stage represents a severe loss of mobility and is the primary outcome that modern treatments aim to prevent.
How often should I do physical therapy?
For the best results, mobility exercises should be performed daily. A structured program usually involves 30-45 minutes of activity, including spinal extension and deep breathing. Consistency is key; studies show that daily engagement leads to a 25-30% improvement in spinal mobility scores over six months.
Why does my back hurt more when I rest?
This is a hallmark of inflammatory pain. Unlike mechanical injury, where rest allows the tissue to heal, inflammatory conditions cause fluid and inflammatory markers to accumulate in the joints during inactivity. This leads to increased stiffness and pain, which only clears once you start moving and "flush" the joints.
